Updated: April 2026
Environmental Health & Safety (EHS) Contacts
EHS Radiation Protection Service
215 Huron Street, 7th Floor
Division of the Vice-President, Research & Innovation
University of Toronto
Toronto, ON M5S 1A2
Operating hours:
Monday – Friday, 9 AM – 5 PM
General Inquiries:
ehs.rps@utoronto.ca
| Name | Position | Contact |
| Research Safety & Compliance – RSC | ||
| Kathy Somers | Executive Director, RSC | kathryn.somers@utoronto.ca |
| Rob Provost | Director Operations, RSC | rob.provost@utoronto.ca |
| Radiation Protection Service – RPS | ||
| Daniel Cardenas | Manager & Radiation Safety Officer | daniel.cardenas@utoronto.ca |
| Vani Ranganathan | Health & Safety Officer | vanieshree.ranganathan@utoronto.ca |
Emergency Contacts
Afterhours, holidays and weekends
| Campus | Emergency Contact |
| University of Toronto – St. George | 416-978-2222 or 911 |
| University of Toronto Scarborough | 416-978-2222 or 911 |
| University of Toronto Mississauga | 905-569-4333 or 911 |
GLOSSARY
ALARA
An acronym for As Low As Reasonably Achievable. The radiation exposure to every person should be kept ALARA, considering social and economic factors
Absorbed Dose
The quantity of radiation energy absorbed in a unit of mass of material. SI unit: Gray (Gy).
Air Kerma
The sum of the initial kinetic energies per unit mass of all the charged particles liberated by uncharged ionizing radiation in air
Background Radiation
Natural radiation resulting from cosmic and terrestrial sources. Background radiation does not refer to occupational exposure or sources from medical uses but includes consumer products
Bremsstrahlung Effect
The creation of X-rays during the slowing down of an electron (or any other charged particle) moving in the strong electric field (e.g.: nucleus field of an atom); this process of X-ray production is called bremsstrahlung from the German phrase “braking radiation”
Characteristic X-rays
X-rays are created when electrons re-arrange inside of an atom, resulting in a loss of energy of the atom in the form of X-rays. This process of emission of X-rays is “characteristic” of the target atom
Dose see Absorbed, Equivalent, or Effective Dose
Dose Rate
It is the dose received per unit of time (e.g.: gray per hour Gy/h, sievert per year Sv/year)
Dosimeter
A device used to record the dose received by an X-ray user. Personal dosimeters (or radiation badges) are worn at chest or waist levels to record whole-body exposure, or on a finger to record the extremity exposure.
Electron Volt (eV)
It is a unit of energy defined as the energy of an electron that has been accelerated through an electric potential of one volt. One electron volt is 1 eV = 1.6 * 10-19 J. Typically the radiation energies associated with X-rays are in order of tens of thousands of eV: 40-80 keV.
Equivalent Dose
A measurement of the biological effects on a tissue or organ exposed to a specific type of radiation. It is a function of the absorbed dose and depends on the type of radiation absorbed. SI unit: Sievert (Sv).
Effective Dose
A measurement of the whole body dose based on the summation of the equivalent dose received by all organs. Each organ contributes with a tissue-weighting factor. The effective dose has the same units of measure as the equivalent dose (Sv).
Exposure
A measure of X-ray intensity in terms of its ionizing effect in air. SI unit: C/kg.
Failsafe Design
A design in which any failure of safety indicators or components that can reasonably be anticipated causes the production or emission of X-ray to cease.
Filtration
A process using filters made from metal to improve the quality of the image obtained with the x-ray machine.
Genetic Effects
Biological effects from ionizing radiation exposure that are inherited by children from their parents
Gray
SI unit of absorbed dose is called Gray (Gy). 1 Gy = 1 J/kg
Ionizing Radiation
Radiation with sufficient energy to create ions, in the context of radiation protection, ionizing specifically refers to the ability to ionize biological tissue
Permit Holder (PH)
Generally, an appointed U of T professor who is the person responsible of an X-ray source situated on U of T controlled areas
Photoelectric Effect
When the interaction between a photon and an atom results in total absorption of the photon and the emission of an electron from the atom. This effect is preponderant at low incident photon energies
Radiation weighting factor
Takes into account the biological effect of each type of radiation on the human body. It is a number between 1 (for beta, gamma and X-ray) and 20 (for alpha or high-energy neutrons) used to calculate the equivalent dose of an organ when the absorbed dose in that organ is know.
Scattered Radiation
When the interaction between a photon and atom results in partial absorption of the photon, the emission of an electron from the atom, and the emission of a scattered photon with lower energy than the incident photon. This effect is also called Compton effect and is preponderant at average incident photon energies.
This term can also be used to describe the X-rays that scatter over and around shielding walls
Sievert
SI unit for equivalent and effective dose (Sv)
Shield or Shielding
Radiation absorbing material used to reduce the absorbed dose or absorbed dose rate imparted to an object or tissue
Somatic Effects
Biological effects from ionizing radiation exposure in our lifetime are called somatic effects. Somatic effects may result from acute or chronic doses of radiation.
Tissue Weighting Factor
Takes into account the biological effect of radiation on different organs or tissues of the human body. It is a percent attributed to each organ or tissue from the human body, used to calculate the effective dose when the equivalent doses received by human organs are known.
X-ray machine
An electrically powered analytical device with the primary purpose of producing X-rays to analyze materials or structures.
X-ray source
Any part of a device, in whole or in part that emits X-rays, whether or not the device is an X-ray machine. The primary use of the device may not be the production of X-rays. Examples include electron microscopes or high voltage sources.
X-ray worker
Any person who in the course of his/her work, business or occupation, is likely to receive a dose of ionizing radiation in excess of the annual dose allowed to the general public.
X-ray source supervisor
An X-ray worker who due to his/her knowledge, experience and training is designated by the permit holder to supervise the safe use of an X-ray source.
X-ray
It is a type of ionizing radiation (maximum energy greater than 5 keV) that is generally produced from machines rather than emitted from radioactive materials. X-rays are made up of photons.
University of Toronto X-ray Safety Program
Preamble
Under its Health and Safety Policy and the general provisions of the Occupational Health and Safety Act (OHSA) of Ontario, the University of Toronto is committed to promoting the health, safety and well-being of its employees, students, visitors, and contractors.
X-ray sources are part of day-by-day university activity. They are present in our research and teaching laboratories, student projects and other activities that incorporate X-ray sources in the educational and research processes. Radiation generated by X-ray sources can cause a wide range of negative health effects when not used following rules and regulations.
The ALARA (As Low As Reasonably Achievable) concept has been adopted by the Institutional Radiation Protection Committee (IRPC) as the philosophy governing the use of all ionizing radiations. The ALARA principle seeks to keep all doses of ionizing radiation as low as reasonably achievable, social and economic factors being taken into consideration. Radiation exposures must be kept below the statutory limit, except for medical radiation exposures. Persons using X-ray equipment should endeavour to keep all radiation exposures as low as possible.
Mandate and Application
The University of Toronto X-ray Safety Program is overseen by the IRPC and implemented by the Office of Environmental Health & Safety (EHS) for the tri-campus community. The University has the responsibility to ensure that reasonable and adequate controls exist for the safe use of X-ray sources in all U of T controlled areas. Hazard evaluations should be performed, and appropriate engineering and administrative controls should be put in place, before using any X-ray sources.
This X-ray safety program applies to areas controlled by the University of Toronto: buildings, structures or open areas, to all employees and students at the University, to occupants of university buildings, and to external organizations that may use or be affected by X-ray sources hazards in such areas.
In the Province of Ontario, the Ministry of Labour, Immigration, Training and Skills Development (MLITSD or traditionally known as the MOL, regulates the use of non-medical X-ray machines under the X-ray Safety Code 861 of the Occupational Health and Safety Act (OHSA). The Ministry of Health (MOH) regulates the use of X-ray radiation on humans (i.e., therapeutic or diagnostic) under the Healing Arts Radiation Protection (HARP) Act. X-ray sources that produce X-rays of high energy capable of inducing radioactivity in exposed materials are regulated and licensed by the federal government under the Nuclear Safety and Control Act (NSCA) and enforced by the Canadian Nuclear Safety Commission (CNSC).
The Institutional Radiation Protection Committee (IRPC)
The IRPC is responsible for the safe use of all sources of ionizing and non-ionizing radiation in all areas at the University of Toronto and is accountable to the Associate Vice-President, Research Oversight and Compliance (AVP-ROC). The use of X-ray sources and X-ray machines is under the jurisdiction of the IRPC and the office of Environmental Health & Safety.
The IRPC approves the University X-ray Safety Program and ensures that all components of the program are adequately implemented. The essential elements of the program are:
- The registration of all X-ray sources used and installed in university-controlled areas with the appropriate regulatory body
- Hazard evaluation of the X-ray sources
- Training of all X-ray sources users
The implementation of these parts of the program relies on university faculty members (Permit Holders/Supervisors) responsible for the use of X-ray sources. The Permit Holders are fully responsible for the safe use of X-ray sources under their jurisdiction. They must ensure that X-ray sources’ users are competent to use X-ray sources safely, that the X-ray sources’ hazard evaluation is performed and that adequate controls are in place, before using the X-ray sources.
Implementation of the X-ray Safety Program
The Radiation Protection Service (RPS) of the Environmental Health and Safety Office has the responsibility of implementing, updating, and auditing the X-ray Safety Program. The AVP-ROC will nominate one RPS staff member as the University X-ray Safety Officer (XSO).
The University X-ray Safety Officer has the authority to stop the use of any X-ray sources in the University controlled areas if the health and safety of persons (faculty, staff, students, visitors) or the environment are at risk. The use of those X-ray sources can be resumed only after all control measures are implemented according to the University X-ray Safety Program and upon written approval of the IRPC.
1. Introduction and Scope
The X-ray Safety Program is designed to maintain effective control of X-ray hazards while ensuring the safety of X-ray users and the general public, while remaining in compliance with applicable laws and regulations governing the use and applications of X-ray radiation and machines at the University.
The basic elements of the X-ray safety program are:
- X-ray permit system;
- registration of all X-ray machines and X-ray sources;
- requirements for the inspections of X-ray machines and X-ray sources;
- requirements for training and education of X-ray workers;
- requirements for personal dosimetry;
- requirements for engineering controls;
- requirements for administrative and procedural controls;
- requirements for reporting accidents/incidents involving X-ray machines and X-ray workers;
- requirements for auditing the implementation and effectiveness of the program.
Scope
This program applies to all X-ray machines and X-ray sources in areas under the jurisdiction of the University of Toronto, including both human and non-human applications. Compliance with this program is mandatory for all faculty, staff or students who possess and/or operator X-ray sources at the University of Toronto.
2. Background & Theory
2.1 Generation of X-rays
X-rays are a type of ionizing radiation (maximum energy greater than 5 keV) that is generally produced from machines rather than emitted from radioactive materials. Gamma and X-rays are not comprised of physical particles like alpha or beta radiation but are made up of individual packets of energy called photons. Unlike gamma rays, which are emitted from the nucleus of a radioactive atom, X-rays are emitted when:
- High-speed electrons (or any charged particles) are slowed down or change direction in a strong electric field like the one created by the nuclei (see Bremsstrahlung Effect) of the target materials. These types of X-rays are called continuous because the x-rays emitted during this process have energies ranging from zero to maximum energy. This maximum energy is equal to the energy of the incoming electron.
- Electrons move from a higher to a lower energy level within the atom. These types of X-rays are called characteristic X-rays and have a line-type spectrum. Therefore, characteristic X-rays are emitted from the electron shell of an atom.
X-rays can also be emitted as a secondary effect in instruments that use high voltages (on the order of tens of kV) as power sources for other applications
2.2 X-ray interaction with matter
After X-rays hit matter they interact with the atoms of the matter through various mechanisms by either being absorbed or scattered. The most common interaction of X-rays with matter include:
2.2.1 Photoelectric Effect
The photoelectric effect occurs when an orbital electron absorbs the energy of an incident photon, and the electron is ejected from the atom. The ejected electron can cause ionization and in the process reduces its energy. This effect is more probable to appear when a low-energy incident photon interacts with a high-Z material target.
2.2.2 Compton Scattering
During this type of interaction, the orbital electron absorbs only a part of the energy of the incident photon and as a result, the electron is ejected from the atom. The remaining energy of the incident photon is carried by a scattered photon. This process is also called Compton scattering. This type of interaction is more probable to occur when the incident photon carries intermediate energy. The scattered photon may undergo another scattering process, resulting in another reduction of energy. When X-rays pass through any material, some will be transmitted, some will be absorbed and some will scatter. The proportions depend on the photon energy and the type of material.
2.3 Units for measuring X-ray energy absorbed in matter
2.3.1 Exposure
X-rays can produce air ionization. The exposure measures the electric charge (positive or negative) produced by electromagnetic radiation in a unit mass of air, at standard atmospheric conditions (STP means 0 degrees Celsius and 760 mm Hg of pressure = 1 atm).
In the SI system of units, exposure is measured in the X unit:
1 X unit = 1 C/kg air
where C stands for coulomb, the SI unit for electric charge.
The average energy dissipated to produce a single ion pair in the air is 34 eV. Since the charge of an electron is equal to 1.6 x 10-19 C, an association can be established between an X unit and the energy measured in joules, dissipated in 1kg of air. Hence, one X unit is equivalent to 34 J/kg.
Exposure refers to the effect of X-rays in air. However, it is often used to characterize the intensity of an X-ray source or an X-ray beam.
2.3.2 Air kerma
Charged particles (free electrons and positive ions) produced by X-rays in the air have each a kinetic energy equal to the difference between the energy lost by the X-rays and the electron bound energy in the atom. Air kerma is the sum of all initial kinetic energies of ions produced by X-rays in a unit of mass of air. The SI unit for air kerma is the same as for the absorbed dose (see below).
Even though the air kerma and absorbed dose have the same units they are quite different. When some of the ions escape from the volume of air (if the air volume is small) air kerma is bigger than the absorbed dose. When all the ions produced are absorbed in the air volume, air kerma is smaller than the absorbed dose
2.3.3 Absorbed Dose (D)
Total X-ray energy absorbed per unit of mass of material is measured in Gy. In this case, the definition is not restricted to air but refers to any type of material.
1 Gy = 1 J/kg
The absorbed dose is used to measure the acute effects of radiation.
2.3.4 Equivalent Dose (H)
The equivalent dose (H) is the physical quantity used to measure the long-term biological effects on a specific tissue or organ. H is a function of the absorbed dose and depends on the type of absorbed radiation. If more than one type of radiation is absorbed in tissue, the equivalent dose, H is:![]()
The radiation-weighting factor (wR) for X-ray is 1 but can vary between 1 to 20 for other types of radiation. H is measured in sieverts (Sv).
2.3.5 Effective Dose (E)
The effective dose, also called the whole-body dose, is the sum of the equivalent doses received by all organs. Each organ that was irradiated contributes to the effective dose with a tissue-weighting factor (WT). WT is expressed as a percentage.
E has the same units of measure as the equivalent dose (Sv)
2.4 Radiation measurements
2.4.1 Particle counting instruments
To measure the intensity of an X-ray source or an X-ray beam a particle-counting instrument can be used. In general, the instruments used to measure X-ray intensity are gas-filled type detectors. This type of detector uses the ionization effect of the X-rays. The most common detectors are Geiger-Muller (GM) or ionization chambers. The meter indication of this type of instrument is in counts per minute (cpm) or counts per second (cps). The reading depends on the type of the detector, the detector’s window and dimensions, as well as on the geometry of the measurement process.
2.4.2 Dose measuring instruments
If a gas-filled detector wall is built with tissue-equivalent material, the instrument can measure tissue dose directly. The most used instrument to measure the exposure or the dose generated by an X-ray source has an ionization chamber detector.
2.4.3 Personal dosimeters
The dose received by a person working with or near an open X-ray source can be measured by a personal dosimeter. There are two different types of personal dosimeters: one that indicates the dose received immediately and one that stores the information inside the dosimeter. In the last case, the stored dose is read later.
A personal electronic dosimeter (PED) is an example of the first type. This instrument can indicate the shallow dose (dose received by the surface of the skin up to the depth of 0.007 cm) and the deep dose (dose received by a person up to one cm depth inside the tissue). It can also be set up to alert, through an alarm system, when a certain dose or dose rate is reached.
A few examples of the second type of personal dosimeters are film, a thermo-luminescent dosimeter (TLD), and optically stimulated luminescence (OSL) dosimeter. The X-ray energy is deposited inside the dosimeter’s material and can be read later by a method specific to each type of dosimeter.
2.5 Biological effects
The biological effects of X-rays can be classified as direct or indirect, acute or delayed, and deterministic or stochastic.
When radiation is absorbed in the biological material causing direct damage to the DNA or other parts of the cell, is called direct action. X-rays can break these molecules and the cell can be damaged resulting in cell death or cell function alteration. The altered cells can be repaired or can be transformed. Depending on the level of radiation the cell death or alterations can be dangerous.
When radiation is absorbed in atoms or molecules other than biological material (for example in a water molecule) the interaction can cause an indirect action. Ions and free radicals resulting from these interactions can damage the biological material indirectly.
Among acute effects of skin overexposure to X-rays are erythema (skin reddening), changes in pigmentation, epilation, blistering, necrosis, and ulceration. Radiation exposure of the whole body with doses between a few hundred mSv and 2000 mSv, can generate acute radiation effects like blood changes, nausea, fatigue, vomiting, impotence, loss of hair, etc. Overexposure of the whole body with a dose of 2000 mSv or more, can result in acute hemopoietic, gastrointestinal, and central nervous system radiation syndromes.
Delayed effects of radiation may be due either to a single large overexposure or continuing low-level overexposures to X-rays. Among the delayed consequences of overexposure to X-rays that are of concern are cancer, genetic effects, mental retardation of children who have been irradiated in utero, and cataracts.
Deterministic effects are effects in which a clear connection can be established between the person that suffered overexposure to radiation and the effect. In these cases, there is a causal relationship between dose and effect on a particular individual. A certain minimum dose must be exceeded to cause a deterministic effect. The severity of the deterministic effects increases with the dose. Deterministic effects can be acute or delayed.
If a large population is exposed to radiation, some individuals will develop cancer and/or damages to the reproductive cells resulting in genetic malformation of the offsprings. These types of effects are called stochastic since they appear by chance. The stochastic effects can occur with no threshold dose, and their probability of occurrence increases with an increase in dose received by the population. The stochastic effects are delayed
3. Roles & Responsibilities
This section outlines the responsibilities for the implementation of the X-ray safety program at the University.
Figure 1: reporting and responsibility structure for the U of T X-ray Safety Program
3.1 Institutional Radiation Protection Committee (IRPC)
The Terms of Reference (TOR) of the IRPC are available on the EHS website.
The IRPC’s responsibilities regarding the X-ray sources are:
- To approve the U of T X-ray safety program; periodically assess its effectiveness and recommend changes;
- To establish and maintain standards and guidelines for the safe use of X-ray sources within the University;
- To provide expert advice on X-ray safety hazards;
- To approve the content of the X-ray safety training;
- To review and act on the recommendation of the Manager, Research Regulatory Affairs and/or X-ray Safety Officer, to suspend, restrict or terminate the operation of X-ray sources;
- To report annually to the AVP-ROC, on the operation of the X-ray safety program.
3.2 EHS Radiation Protection Service (RPS)
The Radiation Protection Service of the office of Environmental Health & Safety has the following responsibilities within the X-ray safety program:
- To update and present the U of T X-ray safety program for approval of the IRPC;
- To nominate one RPS staff member to serve as the X-ray Safety Officer (XSO) to fulfil the requirements of the X-ray safety program;
- To notify Permit Holders of the X-ray safety training requirements of all X-ray supervisors/workers under their authority;
- To provide administrative support to the IRPC regarding the X-ray sources;
- To audit the implementation and effectiveness of this program on an ongoing basis.
3.3 X-ray Safety Officer
The X-ray Safety Officer is reports to EHS leadership and the IRPC and is knowledgeable in the evaluation and control of X-ray sources hazards. The XSO has the following responsibilities regarding X-ray sources in their jurisdiction:
- Hazard evaluation of X-ray sources work area;
- Approval, or recommending for approval, the start of work for new facilities involving the use of X-ray sources, commissioning and decommissioning the X-ray sources;
- Registering X-ray sources used for non-human applications with the MLITSD
- Developing and maintaining policies and procedures for engineering and administrative control of X-ray sources hazards. The XSO is also responsible for ensuring that the prescribed controls are in effect;
- Approval of procedures connected with X-ray sources operation that may be subject to administrative and procedural control;
- Inspection of X-ray sources according to the X-ray safety program;
- Recommendation and approval of protective equipment, X-ray sources working area signs and equipment labels;
- Ensuring safe operation through the authority to suspend, restrict or terminate operations; stopping individual/laboratory work when the safety of workers, the public or the environment is at risk; documenting the technical reasons for the above decision, and reporting to the Director;
- Investigation of the X-ray sources related to incidents and accidents, analysis of the causes, ensuring corrective actions are taken as required;
- Maintenance and updating EHS records, including X-ray sources registrations, inspection reports and training records;
- Prepare, maintain and, when necessary, deliver the appropriate X-ray safety training to all categories of personnel according to the X-ray safety program;
- Verifies the quarterly personal dosimeter reports and investigates all the exposure reports that do not appear to be reasonable and appropriate. The results that are over the regulatory limits will be communicated to the Ontario MLITSD. If a record indicates a value above 0.4 mSv in one quarter and the investigation yields a real result, the XSO will recommend measures to reduce any further exposure;
- Reports on all aspects of the X-ray safety program to EHS senior management as per the reporting structure.
- Providing EHS oversight to clinical and human-participant research X-ray permits
3.4 Facility Radiation Protection Officer (RPO)
For X-ray facilities that use X-ray radiation on human research participants (dental clinic or human research), a qualified Radiation Protection Officer (RPO) who meets the requirements under the HARP Act must be appointed. The RPO is specifically appointed for each facility and has the the following responsibilities:
- ensuring that every X-ray machine operated in the facility is maintained in safe operating condition; and
- such other matters related to the safe operation of each X-ray machine in the facility are as prescribed by the regulations (Ontario Regulation 663/00 – X-ray Safety Code)
- Obtaining and maintaining all appropriate approvals to operate an X-ray source on human research participants from the Ministry of Health (MOH).
- Ensuring X-ray operators using these X-ray sources have adequate training and dosimetry services from EHS and meet the qualification requirements under the HARP Act.
Refer to the Institutional Requirements for Using X-rays on Human Participants for Research Outcomes (Appendix D) for additional information and requirements before engaging in research with X-rays involving human research participants.
3.5 Department Head
The Department Head has the following responsibilities within this program:
- To identify all Permit Holders under his/her authority and ensure that they clearly understand their duties and responsibilities as individuals with principal authority for X-ray sources;
- To ensure that all components of the U of T X-ray Safety Program are implemented in the department.
3.6 Permit Holder (PH)
The PH is a UofT faculty member that is responsible for an X-ray source laboratory and/or principal authority for X-ray sources under their permit. The PH may delegate some or all their responsibilities to an X-ray sources supervisor. However, the Permit Holder cannot discharge these responsibilities to the X-ray sources supervisor.
The PH has the following responsibilities:
- To register all X-ray sources before use, and to deregister the decommissioned ones with the EHS Radiation Protection Service (RPS);
- To be designated as and assume the responsibilities of the “responsible person” for each X-ray source under their permit and as defined by the X-ray regulations of the Ontario Occupational Health & Safety Act, R.O. 1990, Regulation 861;
- To identify all X-ray sources, supervisors and workers under his/her authority to the RPS;
- To ensure that X-ray sources supervisors and workers participate in the University’s X-ray safety program training before operating or working in proximity to any X-ray sources;
- To provide and enforce the use of appropriate personal protective equipment when required;
- To provide and enforce the wearing of a personal dosimeter by all X-ray workers when necessary;
- To provide written standard operating procedures (SOPs) for X-ray sources and to ensure that each X-ray source is used only under conditions and in locations that meet the requirements of the SOP(s);
- To ensure that each X-ray sources supervisor/worker is trained in the safe operation of the specific X-ray sources that he/she will operate;
- To ensure that all X-ray machines and X-ray sources are stored securely and safely when not in use so that they are not usable by unauthorized personnel or under unauthorized conditions;
- To allow only trained X-ray sources supervisors/workers to operate or work in proximity of an open X-ray source;
- To ensure that all administrative and engineering controls are implemented and followed;
- To correct unsafe conditions on time;
- To ensure that all spectators are properly informed of and protected from potential X-ray sources hazards;
- To cancel X-ray sources supervisor/worker privileges until satisfied that he/she fully meets the requirements of this control program;
To report immediately known or suspected accidents to the EHS Radiation Protection Service.
3.7 X-ray Supervisor
The X-ray supervisor is an individual who has been delegated supervisory responsibilities for X-ray sources and X-ray workers by the Permit Holder. The X-ray supervisor has the following responsibilities:
- To participate in the University’s X-ray safety program training before operating or working in proximity to X-ray sources;
- To be familiar with all operational procedures and specific safety hazards of the X-ray sources that he/she will operate/oversee;
- To operate X-ray sources safely and in a manner consistent with safe X-ray sources practices, requirements and written SOPs;
- To operate X-ray sources only under the conditions authorized by the Permit Holder;
- To report all unsafe conditions to the Permit Holder;
- As directed by the Permit Holder, to provide instruction and supervision to X-ray workers;
- As directed by the Permit Holder, to conduct other activities associated with the University’s X-ray safety program;
- To promptly report known or suspected accidents and unsafe conditions to the Permit Holder.
3.8 X-ray Worker
The X-ray worker or user operates or works in proximity to an X-ray source. The X-ray worker has the following responsibilities:
- To participate in the University’s X-ray safety program training before operating or working in proximity to an X-ray source;
- To be familiar with all operational procedures and specific safety hazards of the X-ray sources that he/she will operate;
- To operate X-ray sources safely and in a manner consistent with safe X-ray sources practices, requirements and written SOPs;
- To operate X-ray sources only under the conditions authorized by the X-ray sources supervisor/Permit Holder;
- To report all unsafe conditions to the X-ray sources supervisor/Permit Holder;
- To promptly report known or suspected accidents and unsafe conditions to the X-ray sources supervisor/Permit Holder.
4 Administration of X-ray Machines
4.1 EHS Permit System
4.1.1 X-ray Permit
All X-ray sources and machines in Ontario must be registered with the appropriate regulatory body and under. In addition, all X-ray inventory at the University of Toronto must also be registered and operated under an EHS X-ray Permit. X-ray permits are administered by the EHS Radiation Protection Service and approved by the chair of the IRPC.
X-ray permits typically contain the following information:
- Permit holder name and information
- Approved location(s)
- Approved equipment
- Validity period
- Permit conditions
Any changes to the information on a permit generally constitutes an amendment to the existing permit. PHs should communicate any permit change requests to their Health & Safety Officer.
4.1.2 Permit Eligibility & Requirements
Eligibility
- To be eligible to hold an EHS X-ray permit, holders are required to be full-time University of Toronto faculty members who can supervise daily operations the registered equipment and authorized X-ray users.
- The X-ray permit holder must also act as the “person responsible” for each X-ray source or machine under their permit. The “person responsible” is the individual identified as being responsible for a particular X-ray source or machine at the time of registration.
Permit validity & renewal
- X-ray permits are typically valid from the point of initial approval by the IRPC Chair and expire on the date of expiry of the PHs primary safety training. Permits and training typically expire every three (3) years.
- X-ray permits that remain in good standing may be renewed upon completion of the appropriate refresher training course.
- X-ray permits will not be renewed unless the Permit Holder has completed all required primary training and has met all permit conditions to the satisfaction of the Manager, Research Regulatory Affairs and/or the X-ray Safety Officer.
- An X-ray permit can be considered “out of compliance” if one or more of the permit conditions are not satisfied or if the permit has expired and the permit holder has failed to renew the permit.
4.2 Registration of X-ray Sources & Machines
Depending on the specific application, X-ray machines and sources must be registered with either the Ministry of Labour, Immigration, Training and Skills Development (MLITSD) or the Ministry of Health (MOH). Registration applications for X-ray machines not used on humans are submitted by EHS on behalf of the permit holder. X-ray machines used on humans for research or clinical purposes are registered by the Facility Radiation Protection Officer (RPO) with EHS guidance. General registration procedures and requirements are provided in the following sections.
4.2.1 Registering cabinet, mobile and open-beam X-ray sources
There are two primary reasons for preparing and maintaining a record of all X-ray sources. These are:
- To identify areas where X-ray sources are present so that appropriate administrative and engineering controls may be put in place;
- To enable the X-ray sources to be inspected regularly for compliance with the University’s X-ray safety program.
The Permit Holder is responsible for the registration of all X-ray sources and the deregistration of decommissioned ones (see the X-ray Permit Application form in Appendix A).
The PH shall request a review of the approval if, after the installation of an X-ray in a permanent location, there is a change in:
- The position or use of the X-ray source;
- The use of the rooms or areas adjacent, horizontally or vertically, to the X-ray source, or
- Any shielding of the X-ray source.
Any of these changes may increase the exposure of faculty, staff, students or visitors.
An X-ray source may be portable or mobile for the purpose if its use. Approval from the MLITSD must be obtained by RPS for the mobile use of an X-ray source. The XSO is responsible for the preparation and maintenance of the internal X-ray sources registry with the MLITSD.
4.2.2 Registration of X-ray Fluorescence (XRF) sources
- The MLITSD requires certification of all X-ray owners and operators using an XRF analyzer from the Natural Resources Canada (NRCan) National Non-Destructive Testing Certification Body (NDTCB).
- EHS will not submit X-ray applications to the MLITSD without the necessary certification(s)
- More information regarding the certification process can be found here: https://www.nrcan.gc.ca/science-and-data/non-destructive-testing/about-certification-ndt/apply-xrf-analyzer-operator-certification/19583
4.2.3 Registration of X-ray sources for use on Humans
Any X-ray machine or source used on humans must be registered with the Ministry of Health (MOH) by the facility RPO and must meet the requirements outlined by the HARP Act and Regulation 543, including but not limited to:
- Written approval is required prior to machine installation from the MOH (Section 3 of the HARP Act)
- There must be a qualified individual operating the X-ray machine (Section 5 of the HARP Act)
- The irradiation must be prescribed by a qualified individual (Section 6 of the HARP Act)
- There must be a qualified individual designated as the Radiation Protection Officer (RPO) for the facility where the X-ray machine is installed (Section 9 of the HARP Act)
- The X-ray machine must undergo testing immediately after installation and subsequent periodic testing (Section 8 of Reg 543)
Additionally, X-ray machines or sources used on humans for research purposes must meet all the requirements outlined in Appendix D.
5 X-ray Safety Inspections
Periodic inspections of X-ray sources are an integral part of the X-ray safety program; inspections provide some indication as to whether or not these X-ray sources are being operated safely. The X-ray safety inspection checklist is presented in Appendix C. The PH will be informed about the results of the inspection (a copy of the checklist will be sent to the PH) and of the necessary measures to improve the safe use of the X-ray source.
The XSO is responsible for inspecting all X-ray sources on University of Toronto property on an annual basis in order to maintain compliance with the University’s X-ray safety program. The XSO is also responsible for providing reports to the Radiation Protection Service (EHS) and the IRPC.
6 Safety Training Requirements
Primary safety training
All X-ray permit holders, X-ray supervisors and X-ray workers must participate in the University’s X-ray safety training before operating or working in the proximity of X-ray machines or sources. Safety training courses are offered online and address the following topics:
- X-ray basics;
- X-ray hazards, bio-effects;
- Engineering and administrative control measures;
- X-ray safety regulations and U of T X-ray safety program;
- Responsibilities of personnel;
- Causes of accidents;
- X-ray accident reports;
Refresher training
All persons operating an X-ray machine or source shall participate every 3 years in the refresher training sessions organized by the RPS. The refresher training typically includes:
- X-ray safety updates;
- Changes in X-ray safety legislation;
- Changes in U of T X-ray safety program;
- Responsibilities of personnel;
- Results of X-ray safety inspections;
All courses are followed by an evaluation; participants must achieve a passing grade of 80%. The EHS XSO and Radiation Protection Service is responsible for maintaining records of all X-ray supervisors and X-ray workers who have participated in the X-ray safety program training and for notifying Permit Holders of this participation.
Other training considerations
- All X-ray supervisors must also be familiar with all standard operating procedures and specific safety hazards of the X-ray machines that they will operate/oversee.
- All X-ray workers must also be familiar with all standard operating procedures and specific safety hazards of the X-ray machines that they will operate.
- To use handheld XRF devices, the X-ray worker needs to obtain the appropriate certificate of the Natural Resources Canada (X-Ray Fluorescence Analyzer Operator Certification) before registering or operating a handheld XRF device.
Training Records
All EHS training records are maintained in the EHS data management system, SPROUT. Participants in EHS courses must obtain a passing grade for their training record to be reflected in SPROUT.
List of X-ray safety training courses
The EHS Radiation Protection Service offers a variety of X-ray safety courses tailored to specific applications. A summary of the courses is provided below:
| Course Code | Name & Description | Required for |
| EHS 741 | X-ray SafetyThis course is designed for all personnel operating or working with X-ray sources |
|
| EHS 742 | X-ray Safety – Faculty of DentistryThis course is designed for permit holders and operators of clinical X-ray machines at the Faculty of Dentistry only. It is also recommended for personnel working near clinical X-ray machines. |
|
| EHS 743 | X-ray Safety – Human Research ApplicationsThis course is designed for permit holders and operators of clinical X-ray machines that are used for human research applications. It is also recommended for the facility RPO. |
|
| EHS 745 | X-ray Safety RefresherThis course is a condensed version of the primary X-ray safety course. Personnel working with or operating X-ray sources must complete this course every three (3) years |
|
7 Accident/Incident Reporting and Emergency Response
The University’s health and safety policy requires the reporting of all accidents/incidents, which result in or have the potential to result in a personal injury.
Reporting of accidents involving death, critical injury, lost time or health care is required for employees under the Occupational Health and Safety Act and the Workplace Safety and Insurance Act, while University policy requires the reporting of accidents/incidents involving students and visitors and other persons on university premises.
Therefore, reportable accidents/incidents are those which:
- Result in personal injury (including those requiring first aid) or property damage; or
- Have the potential to result in significant personal injury or property damage even though no injury or damage occurred; and
- Occur to any person on university premises; or
- Occur to a university employee during his/her work either on or off university premises.
The Permit Holder is responsible for reporting all accidents/incidents involving X-ray sources:
- For incidents involving employees, students, visitors and others, the Permit Holder must submit an Accident/Incident eForm
Where an X-ray worker has received in one quarter a dose above the annual limit (5 mSv for whole-body exposure of 50 mSv for any individual organ) set out in Column 4 of the Schedule of X-ray Safety Code R.R.O. 1990, Reg. 861, the XSO will investigate the cause of exposure and will provide a report in writing to the Director of Ministry of Labour, Immigration, Training and Skills Development (MLITSD) and the Joint Health and Safety Committee of the findings and of the corrective actions taken.
When an accident, failure of any equipment or other incident occurs that may have resulted in a dose received by an X-ray worker is more than the annual limit (50 mSv for whole-body exposure, 150 mSv for the lens of the eye exposure, or 500 mSv for any other individual organ) set out in Column 3 of the Schedule of the Ministry of Labour X-ray Safety R.R.O. 1990, Reg. 861, the PH will notify immediately the Office of Environmental Health and Safety (EHS). EHS will inform, by telephone, or other direct means the Director of Ministry of Labour, Immigration, Training and Skills Development and the Joint Health and Safety Committee. The PH should also send to the EHS a written report of the circumstances of the accident or failure. EHS will send this report to the Director of the Ontario MLITSD.
All reportable accidents/incidents must be reported to EHS within 24 hr so that the appropriate report is filed with the Workplace Safety and Insurance Board.
When a known or suspected accident is reported to the Permit Holder/X-ray sources supervisor or the Office of Environmental Health and Safety, the X-ray sources worker with a suspected injury will be referred to the appropriate University Health Service or hospital.
8 Dosimetry Program
8.1 Personal Exposure Monitoring
All X-ray workers, supervisors or PHs working with, or within the vicinity of, an open beam X-ray source shall wear whole-body and ring personal dosimeters. If the door of a cabinet X-ray machine is open, the interlock is bypassed for repair, maintenance or beam alignment, the X-ray source must be considered an open beam system.
Dosimeters can be requested from RPS using the “Dosimeter Request Form” available on our website or in Appendix B. If the X-ray source is enclosed in a cabinet, no radiation dosimeter is required. A Canadian Nuclear Safety Commission (CNSC) certified dosimetry service should be used to provide the dosimetry service for the U of T.
The XSO will verify that the dose recorded by the personal dosimeter is reasonable and appropriate in the circumstances and will notify an inspector of the Ontario MLITSD of any dose that is above the regulatory limits.
The RPS will retain the personal dosimeter records for 3 years. The National Dose Registry of Health Canada keeps lifetime exposure records.
If, when using an X-ray machine for the diagnostic examination of animals, the animals are required to be held by a hand, a protective apron and gloves providing shielding equivalent to at least 0.5 mm of lead shall be worn by the person providing the restraint or support. The person shall wear an extremity dosimeter (ring) under the gloves during the procedure. It is forbidden to hold the film cassette by hand. A record of radiographic exposures, including the date, kilo-voltage, tube current, and duration of each exposure shall be maintained and kept for at least one year.
Each declared X-ray pregnant worker will be provided with a Personal Electronic Dosimeter (PED). The weekly readings of the dosimeter will be communicated to the XSO at the end of each working week. Any unusual reading and anytime alarm sounds will be communicated to the RPS immediately.
8.2 Dose Limits and Action Levels
Occupational exposure to X-ray radiation by worker in Ontario is governed by the Occupational Health and Safety Act (OHSA). Occupational exposure limits for the X-ray workers and other workers can be found in table 1.
The MILTSD does not set out an investigation level. However, the institutional investigation level set out by the U of T X-ray safety program is 0.4 mSv in a quarter (3-month monitoring period) in alignment with the U of T Radioactive Materials Program. If this level is reached an automatic investigation is triggered and must be conducted by the XSO. The XSO will determine the manner and circumstances that led to the worker receiving a dose at or above the program investigation level and will consult with the worker and their supervisor how to reduce occupational exposure. Actual dose limits for workers set out by OHSA are shown below in Table 1.
Table 1: Dose limits for workers set out by the OHSA, RRO 1990, Reg 861.
| Part of body irradiated | Exposure conditions and comments | Dose equivalent annual limit (mSv) | |
| X-ray Workers | Other Workers | ||
| Whole body or trunk of body | Uniform irradiation | 50 | 5 |
| Partial or non-uniformIrradiation of body | The limit applies to the EFFECTIVE DOSE EQUIVALENT defined in Note (a) | 50 | 5 |
| Lens of eye | Irradiated either alone or with other organs or tissues | 150 | 50 |
| Skin | The limit applies to the mean dose equivalent to the basal cell layer of the epidermis for any area of skin of 1 square centimetre or more | 500 | 50 |
| Individual organs or tissues other than lens of eye or skin | The limit on effective dose equivalent applies, with an overriding limit on the dose equivalent to the individual organ or tissue | 500 | 50 |
9 Hazard Control and Radiation Protection
Evaluating the hazards and implementing appropriate administrative and engineering controls are an essential part of the X-ray safety program.
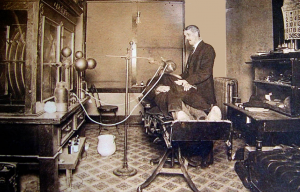
Fig. 9.1: X-ray Safety in the early 1900s
As can be seen in Fig 9.1 at the beginning of the general use of X-ray machines in diagnostics and treatments, there was no control of the x-ray hazards. The physician is exposed to as much radiation as the patient. But since the patient is exposed only when necessary and the physician is exposed with every patient, the total dose received by the physician is much larger. The negative long-term effects of radiation exposure were unknown. A few decades later (the early 1920s) many physicians start dying from cancer. This triggered the creation of the International Commission of Radiation Protection (ICRP).
9.1 X-ray Hazard Assessment
The first step in X-ray hazard control is hazard assessment. The hazard assessment is performed by the X-ray Safety Officer (XSO). The work supervisor (in most university’s laboratories the work supervisor is a University Professor) must inform the XSO by completing and submitting the form from Appendix A (see also chapter 4 of this document). The EHS Radiation Protection Service must apply to register the X-ray machine with the Ontario MLITSD.
The XSO will visit the laboratory to confirm the information received, estimate the radiation hazards and measure the radiation leaks. Considerations for different types of hazard assessments are provided below.
9.1.1 Closed Beam X-ray Machines
An X-ray machine used for sample analysis is considered enclosed in a cabinet if:
- The enclosure provides sufficient shielding to ensure that the radiation exposure at any accessible point of the external surface is under 2.5 µSv/h
- The cabinet’s door is lockable and cannot be opened if the X-ray beam is not blocked
- The cabinet walls cannot be removed without using adequate tools
- The door and any removable part/walls of the enclosure must have interlocks installed
- If the cabinet door or any part of the enclosure are open when the X-ray is not blocked, the interlocks must stop the operation of the X-ray tube
- The X-ray machine must restart from the control panel or computer only when the door or removable walls are closed and interlocks are functional
- The control panel (or the computer used to control the machine) must be situated outside of the cabinet and must indicate the voltage and the current
- The cabinet must have radiation warning labels
- The light indicating that the x-rays are emitted must be visible
9.1.2 Open Beam X-ray Machines
Open beam X-ray machines are usually used in animal facilities, dentistry, and clinics. Sometimes low high voltage and current X-ray machines are used in mobile open beams x-ray machines for sample analysis (geological samples, small animals, etc.) in the field.
If an open beam X-ray machine is used in a permanent location, the entire room will be considered a controlled X-ray zone. Access to the room must be restricted to authorized personnel, the door must have a lock and an interlock. A warning light must indicate the condition of the shutter (open or closed). Area dosimeters may be required in addition to personal dosimeters.
9.1.3 Fixed and mobile X-ray Machines
X-ray machines used in a permanent location can be enclosed in a cabinet or open beams. They must be recorded with the Ontario MLITSD as fixed X-ray machines. The mobile X-ray machines have lower high voltage and current and are open beam. They are used to analyze the sample composition in the field.
The mobile X-ray machines are registered with the Ontario MLITSD as mobile X-ray machines and can be used anywhere in the Ontario province. If a mobile X-ray machine is used outside Ontario, it must be registered within the province or territory before can be used in that province or territory.
9.2 Engineering Controls
Engineering controls are physical barriers designed to keep the risks of using X-ray sources under control. When, due to the nature of the device these engineering controls are not applicable, the PH must ensure that equivalent controls are in place. These controls should offer equal or greater protection than the ones described here.
9.2.1 Shielding
To reduce the dose received by X-ray workers according to ALARA and under the permissible limits, structural or another shielding shall be installed as is necessary
The XSO will assist in calculating the thickness of the shielding for each application as required.
If a lead apron and gloves are required when using an X-ray machine, the material will provide a shielding equivalent to at least 0.5 mm of lead.
9.2.2 Diaphragms, Cones, Collimators
Diaphragms, cones and adjustable collimators or other suitable machines shall be provided and used as are necessary to limit the dimensions of the useful X-ray beam.
Each port shall be designed in such a way that the X-ray beam can emerge only when a camera or other recording machine is in its proper position, wherever applicable.
All unused ports shall be secured in such a way as to prevent inadvertent opening.
9.2.3 Locks, Interlocks
When the radiation exposure in an area may exceed 25 µSv/h access to the area should be controlled by:
- Locks or interlocks if the X-ray source is installed in a permanent location;
- Barriers and X-ray warning signs if the X-ray source is portable or mobile and is being so used;
- A guard or interlock which prevents entry of any part of the body into the primary beam path shall be used, wherever applicable.
When an interlock terminates an exposure, it shall only be possible to restart the exposure from the control panel.
9.2.4 Shutters
A shutter is a mechanical device installed near the exit of the X-ray tube capable of blocking the beam when it is necessary. The shutter may be used in connection with an interlock to stop the beam.
9.3 Administrative and Procedural Controls
Engineering controls must be given primary consideration in instituting a control measure program for limiting access to X-ray sources radiation. If some of these engineering controls are impractical or inadequate, then administrative and procedural controls that provide equivalent protection shall be used.
Administrative and procedural controls are methods or instructions which specify rules, or work practices or both, which implement or supplement engineering controls and which may specify the use of personal protective equipment.
The following are guidelines for the safe use of all X-ray equipment in general:
- The equipment shall be used under the guidance and supervision of a qualified person who is also responsible for the safe use of the equipment.
- X-ray warning signs shall be posted on the doors of all X-ray rooms, and X-ray warning labels shall be affixed to all X-ray equipment.
- All work should be well planned before carrying out an experiment or making an exposure.
- Persons who are classified as X-ray workers shall all wear personal dosimeters, as provided by their respective departments.
- Persons wearing lead aprons should wear their dosimeter under lead aprons to avoid false high readings.
- All equipment capable of producing X-rays shall be lead shielded or installed in a protective lead enclosure. The area in which this equipment is used shall be marked with warning signs to indicate that x-radiation may be present.
- Energized equipment shall not be left unattended in a location with unrestricted access.
- High voltage power supplies using rectifier tubes should be housed in protective lead enclosures.
- The latest Leakage Certificate should be posted in the approved space(s) for each active X-ray machine.
- A radiation survey of a new or modified X-ray installation and its vicinity shall be carried out before it is put into operation, to ensure compliance with regulatory requirements.
- Protection of staff or students working in areas surrounding an X-ray machine should be achieved by using lead barriers, which absorb the scattered, leakage, or transmitted radiation. The barriers shall be positioned as close as possible to the equipment.
- The primary beam shall be directed towards an unoccupied area (i.e. an area to which access is not permitted) or towards a wall containing adequate shielding. The beam should be well collimated so that it covers only the minimum area necessary for the nature of work being undertaken.
- Protective lead aprons and gloves shall be inspected annually to ensure that they remain in good condition.
- A mobile X-ray machine used routinely in one location should be considered as a permanent installation and be lead or lead equivalent shielded accordingly.
- Before any major change/modification of the approved X-ray installation, or the use of the X-ray machine, which may increase the exposure of the machine user, an application shall be prepared and submitted to the appropriate Ministry through the Radiation Protection for Ministerial re-approval.
- Early submission to the Radiation Protection Service for any new project using an X-ray tube for proposed research or experiment would ensure that any problems could be considered and discussed in advance. A radiation survey shall be carried out before the X-ray work.
- The Radiation Protection Service shall be provided with written notice in advance of any purchase of new X-ray equipment, or the sale, relocation or disposal of an existing X-ray machine or source.
- The X-ray tube shall not be energized during adjustments or repairs or when any protective safety cover is removed.
- No interlock or other safety device shall be deliberately defeated or bypassed.
- Any defect in a piece of X-ray equipment shall be reported immediately to the authority responsible for the radiation safety of the equipment and to the Radiation Protection Service.
- Service specialists, such as the manufacturer’s agents will normally carry out repairs, etc. When internal University personnel are used, their competence to control any radiation hazard incidental to the repair procedure, and the use of the repaired equipment, shall be established before initiating the repairs.
9.3.1 Standard Operating Procedures (SOPs)
Standard operating procedures (SOPs) for X-ray machines shall be kept close to the X-ray machine and must always be available as a reference for all X-ray workers; SOPs may include the X-ray sources instruction manual (prepared by the manufacturer) and as appropriate, additional written information to ensure compliance with good work practices and safety.
The SOP must contain information about the X-ray machine (manufacturer, model, serial number, maximum high voltage and current), and the list of authorized personnel.
In addition to the above information, typical examples of SOPs for the X-ray machines used in our university must contain the following information based on the X-ray machine usage.
9.3.1.1 Cabinet X-ray Machine Used for Sample Analysis
- A visual inspection of the signage, functioning of the warning light and integrity of the cabinet must be performed every time before operating the X-ray machine
- Perform the mandatory operation required by the operation manual/instructions given by the manufacturer for starting the X-ray machine
- Prepare and insert the sample in the sample holder
- Close the door and start the measurement
- To change the samples the X-ray machine must be stopped
- After putting the new sample the door must be locked
- At the end of the work the X-ray machine must be closed and the key must be removed. Only authorized personnel must have access to the key
- No radiation badges are required when operating a cabinet analytical X-ray machine
If the interlocks must be bypassed for repair/calibration/alignment the X-ray machine will be considered an open beam X-ray machine. These operations must be performed by a trained X-ray worker wearing a whole-body and a ring radiation dosimeter.
9.3.1.2 Open Beam X-ray Machine Used for Sample Analysis
- Establish the area where the radiation field is above 2.5 µSv/h
- Mark the area with radiation signs and control access to the area by using physical barriers or tape indicating radiation danger. Only persons from the authorized user list are allowed inside the area
- All persons inside the controlled area must wear whole-body radiation dosimeters
- An authorized user must be present when the X-ray is operational
- If the operator must be in an area where the radiation field is above 25 µSv/h, a lead barrier must be used to reduce the exposure under 25 µSv/h
- Perform the mandatory operation required by the operation manual/instructions given by the manufacturer for starting the X-ray machine
- The X-ray emission must be stopped when inserting or changing the sample
- At the end of the work the X-ray machine must be closed, and the key must be removed. Only authorized personnel must have access to the key
9.3.1.3 X-ray Machines Used for Animal Diagnosis
- Only persons with adequate X-ray safety and animal safety training are allowed to use X-ray machines on animals
- An X-ray controlled area must be established through walls, doors, physical barriers and marked with radiation warning signs. A warning light must indicate when the X-rays are emitted
- The radiation exposure outside the X-ray controlled area must be under 2.5 µSv/h
- Access to the X-ray controlled area must be permitted only to authorized personnel
- The X-ray machine operator must be outside the X-ray controlled area.
- If possible, the animal must be sedated and no person shall be present in the X-ray controlled area where the operation is performed
- If a person is required to be inside the controlled area to assist the operation by holding the animal, the person must be designated as an X-ray worker, wear a lead apron, lead gloves, and whole-body and ring radiation dosimeters
- Any part of the body of the person must be kept outside the main beam
- The person must never hold the radiography film by hand
- At the end of the work the X-ray machine must be closed and the key must be removed. Only authorized personnel must have access to the key
9.3.1.4 Procedure for Using Dental X-ray Machines
In addition to the relevant precautions set out in previous sections, the following rules shall be observed in using X-ray emitting machines for dental diagnosis:
- In operating an X-ray machine for diagnosis, students or persons in training shall work under the direct supervision of an experienced operator authorized by the person in charge of the department. They shall not be allowed to irradiate patients until they have received sufficient instruction in the precautions necessary for the safe operation of the equipment.
- The X-ray exposure should be controlled only from a lead shielded control booth where the patient can be observed through a viewing window having lead-equivalent thickness conforming to the rest of the shielding.
- Control knobs for adjusting kilovoltage, milliamperage, power-on, or X-ray-on switches shall have their functions clearly and durably labelled.
- All pilot lights, which indicate that the control panel is ready to be energized, shall be ON
- The X-ray tube shall be rigidly fixed and correctly aligned within its tube housing. The tube head shall maintain its exposure position without drift or vibration during the examination.
- Lead-lined localizing collimators or cones shall be used with all dental equipment. Such collimators or cones shall provide the maximum practical field size in conformity with the requirement set by the government, or other regulatory agencies.
- Open-ended cones shall be used for intraoral examinations.
- The equipment shall be provided with an automatic timer, which will terminate the exposure after a preset time or earlier at the discretion of the operator.
- The X-ray tube housing or cone shall not be held by hand during exposure.
- No person other than the intended patient may place any part of his or her body in the direct beam.
- Dental films shall be placed in a fixed position. If the patient is a child or in a weak condition, the film can be held by an accompanying adult who is suitably protected. Under no circumstances may the film be held by a person occupationally exposed to x-radiation.
- Gonadal lead shielding and, when appropriate, thyroid lead shielding shall be provided for all X-ray exposures on children and persons of reproductive age.
- The exposure of the patient during an X-ray examination shall be kept to a minimum necessary to produce satisfactorily diagnostic results.
- An X-ray room in which more than one open X-ray machine is installed shall not be used for more than one X-ray measurement at any one time unless an appropriate barrier has been installed to ensure adequate separation and protection.
- Where more than one tube is controlled by one control panel, dental X-ray equipment shall be designed to facilitate the inclusion of an interlock system such that it is not possible to energize more than one tube at a time, and an indicating light will show which tube is connected and is ready to be energized.
To avoid an excessive number of duplicated exposures, the processing of exposed films should be as specified by the X-ray manufacturer.
9.3.1.5 Procedure for Using X-ray Machines on Persons
In addition to the relevant precautions set out in the previous sections, the following rules shall be observed in using radiographic equipment on persons/patients:
- No person shall operate an X-ray machine for the irradiation of a human being unless the operator meets the qualifications and requirements as outlined in the Healing Arts Radiation Protection Act (HARP), and authorized by the individual in charge of the X-ray facility.
- The entrance door to the X-ray room should be kept locked during all exposures.
- Where possible, X-ray exposure shall be controlled only from the lead shielded control booth.
- X-ray radiation warning signs forbidding unauthorized use shall be affixed to the control panel of the equipment.
- The beam exposure switch should be of the fail-safe type in which the power is turned off immediately upon release of the switch.
- The total filtration should be permanently installed in the X-ray machine.
- The X-ray tube shall be mounted in lead shielded type housing.
- The equipment shall be provided with collimating devices to keep the size of the primary beam equal or less than the area of the X-ray film selected for each exposure.
- Quality assurance testing for the medical X-ray machine used for patient diagnostic purposes must be carried out following the regulatory requirements set out by R.R.O. 1990, Regulation 543.
9.3.2 X-ray Worker Training
Education and training shall be provided for all X-ray workers (see section 6 of this program). The level of training shall be commensurate with the level of a potential hazard.
9.3.3 Authorized Personnel
X-ray sources shall be operated, maintained or serviced by authorized personnel. Authorization to operate, maintain or service an X-ray machine is given by the PH responsible for the X-ray machine. If authorization is given to an external contractor, the PH must verify the qualifications and the records of X-ray safety training of the contractor and inform the RPS. The XSO will verify the list of the authorized person to confirm that the person/persons have the appropriate training.
9.3.4 X-ray Signs and Warning Signals
The general requirements for signage and hazard awareness for X-ray machines/sources and X-ray facilities are as listed below:
- Each room that has an X-ray source must have visible signs on all doors indicating that this is an X-ray room.
- Each X-ray source shall have the appropriate signs indicating that X-rays are being produced and that moving of the X-ray source to a different room must be communicated to the RPS.
- The control panel should indicate when the X-ray machine is producing X-rays.
- A warning light shall be mounted near each X-ray machine in such a way as to be visible from any direction from which the X-ray machine can be approached, which indicates when X-rays are being produced.
- The status of each shutter, open or closed, shall be indicated at or near the X-ray tube.
- In the case of cabinet X-ray equipment, the warning signal should be mounted on or near the cabinet in such a way as to be noticeable from any position from where the cabinet can be opened.
Cabinet X-ray equipment that is intended to allow the entry of a person shall also be provided with:
- Suitable audible or visible warning signals within the cabinet that shall be actuated for at least 10 seconds immediately before the initiation of X-ray production after the closing of any door that is designed to allow human access into the cabinet;
- Suitable audible or visible warning signals within the cabinet that shall activate during X-ray production;
- Effective means within the enclosure to prevent or interrupt the production of X-rays, that cannot be reset from outside the enclosure and that can be reached without having to pass through the primary X-ray beam.
9.3.5 Leakage Surveys
The EHS Radiation Protection Service conducts regular leakage surveys of scattered and leakage X-ray radiation from all registered X-ray machines and/or sources to ensure exposures are below 5 µSv/hour 5 cm from any surface of an X-ray machine, as per the X-ray Safety Code, R.R.O. 1990, REGULATION 861. An X-ray Leakage Certificate for each machine will be issued and must be posted in all the permitted space(s) on the X-ray permit.
9.4 Personal Protective Equipment
If the X-ray machine is enclosed in a locked cabinet and the radiation leak measurements confirm no radiation dose above the background, the users do not need X-ray protective equipment. They may need the lab coat, gloves and goggles for chemical or biological safety depending on the nature of the samples handled.
For open beam X-ray machines, lead aprons, lead gloves or appropriate protective equipment may be required to reduce the level of irradiation from direct or scattered X-ray radiation. The personal dosimeters (whole body and ring, if required) will be worn under the lead apron or gloves to eliminate unreasonable dose recordings by the dosimeters.
A protective lead apron and gloves are required to be used when an X-ray machine is used for the diagnostic examination of animals, and the animals are required to be held by a hand. The lead equivalent of the protective apron and gloves must be at least 0.5 mm of lead. The body and the hand of the person must be outside of the X-ray main beam. It is forbidden to hold the X-ray film by hand. Dental patients must be protected by a lead apron. The dental technician using the X-ray dental machine must be outside the room when the X-ray is ON.
At a minimum, a visual inspection of lead protective equipment (e.g., aprons, gloves, skirts) must be performed every time before using them. Radiographic testing of lead protective equipment can also be performed. The visual and/or radiographic inspection must identify any tearing or bending of the material that may result in leakage or uneven exposure to X-ray radiation. Defective protective equipment must never be used.
The XSO must inspect the condition of the personal protective equipment during the X-ray safety inspections (see chapter 5 of this document).
10 Program Audit
components of the X-ray safety program on an annual basis and prepare a report to the IRPC.
The audit may consist of but is not limited to the following:
- Inspections of some X-ray sources facilities for compliance with the University’s X-ray safety program;
- Review of training records to confirm that X-ray sources supervisors/workers have had appropriate training to work with X-ray sources;
- Review of records vs. inspections to confirm that the registration/deregistration process is working effectively.
- Review of program policies and procedures to reflect changes in regulatory requirements or operational needs
- Review the relevancy and applicability of our training courses
A Joint Health and Safety Committee may, as part of its inspection of the workplace and subject to access control procedures, inspect X-ray sources facilities.
11 X-ray Permit Termination and Disposal of X-ray Machines
The EHS Radiation Protection Service must be informed in writing when the installation is no longer to be used for X-ray work or when an X-ray machine is to be transferred or decommissioned.
If the X-ray machine is transferred to a different permit holder or a different institution RPS must be informed about the name and address of the new owner.
The following procedure must be followed for the disposal of X-ray equipment.
For the disposal of an X-ray machine, the XSO shall observe the instructions provided by the manufacturer in the product manual or contact the manufacturer for information and guidance. In a case where a manufacturer is no longer in the business of manufacturing, selling or servicing industrial X-ray equipment, the following procedures shall be followed:
- the vacuum in the X-ray tube must be breached;
- the X-ray tube window should be inspected to determine whether or not it contains beryllium, and if it does, special disposal procedures must apply since beryllium presents toxic ingestion or inhalation hazards;
- the transformer oil, if this exists, must be disposed of following pertinent environmental legislation; and
- the lead must be recycled accordingly
If no other X-ray source remains under the supervision of the PH, the X-ray permit will be archived by the RPS.
12 References
- Occupational Health and Safety Act, X-ray Safety R.R.O. 1990, Regulation 861, Ontario Ministry of Labour
- Healing Arts Radiation Protection Act, Ontario Regulation 663/00 X-ray safety Code Ontario Ministry of Health
Appendix 1 – X-ray Permit Application form
The form to completion can be found in X-Ray Permit Application (PDF).
Appendix 2 – X-ray Training and Personal Dosimetry Form
The form can be found at: Radiation Badge Application Form (PDF)
Appendix 3 – X-ray Safety Inspection Checklist
University of Toronto – Radiation Protection Service |
||||||
Environmental Health and Safety |
||||||
Analytical X-ray Equipment Inspection Report |
||||||
| Permit # | Revision # | |||||
| Principal Investigator | Department | Date | ||||
| Building | Room # | RSO | ||||
| Equipment | ||||||
| Manufacturer | Type | Max kV | ||||
| Model | Serial # | Max mA | ||||
| Code | Description | Y / N | Comments | |||
| A02 | Lab not listed in the appropriate permit | |||||
| A03 | Entry door to lab is not lockable or the lock is not working properly | |||||
| A06 | Lab worker not attached to the corresponding permit | |||||
| A07 | Worker has not taken the required training course | |||||
| A55 | Gas cylinders are not secured at ~ 2/3 their height in an upright position or in an bolted floor mounted apparatus | |||||
| X01 | Current X-ray permit not posted | |||||
| X02 | Drawing approved by MOL not posted | |||||
| X03 | List of authorized X-ray users not posted | |||||
| X04 | Room X-ray sign not posted | |||||
| X05 | X-ray source sign not posted | |||||
| X06 | “Do not move the equipment” sign not posted | |||||
| X07 | UofT Emergency Numbers not posted | |||||
| X08 | Access to X-ray source is not controlled | |||||
| X09 | Unattended labs are not locked | |||||
| X10 | Unattended X-ray sources are not locked | |||||
| X11 | Current SOPs are not posted by the X-ray machine/source | |||||
| X12 | X-ray source not periodically inspected by X-ray supervisor | |||||
| X13 | X-ray source leakage not checked | |||||
| X14 | Appropriate shielding is not available | |||||
| X15 | X-ray machine key control not used | |||||
| X16 | X-ray tube ON warning light not functional | |||||
| X17 | ON/OFF X-ray tube energized sign on control panel not functional | |||||
| X18 | Diaphragms, cones and collimators are not provided if necessary | |||||
| X19 | Primary beam not terminated | |||||
| X20 | Unused port flap shutter not installed | |||||
| X21 | Cabinet/shield/sample interlocks not installed | |||||
| X22 | Interlocks are not functional | |||||
| X23 | Dose rate does exceed 5 μGy/hr (0.5mR/hr) at 5 cm from cabinet | |||||
| X24 | TLD badge not worn if required | |||||
| X25 | Improper TLD storage when not in use | |||||
| X26 | Lead apron or gloves not available or not worn if necessary | |||||
| X27 | UofT X-ray Safety Manual is not available to all users | |||||
| X28 | Principal Investigator or designate not available to supervise | |||||